I always wonder what more could have been done for Ms Harry*.
Ms Harry was an Indigenous Elder and a patient in my practice who was more focused on the community than on caring for her own health, especially as related to her diabetes. She died in her 50s from a myocardial infarction, unexpectedly and before we were ready for her to leave us.
Ms Harry’s premature death left me wondering—what if we managed her diabetes better? What could I, as her physician, have done differently?
All clinicians have patients who affect us this way. It may have been a patient with cancer, heart failure, or even a mental health or social issue that makes us question what we could have changed or improved in their care. These patients stay with us.
It’s often difficult to think beyond the care of a single patient. We think about the management of an individual and apply care based on that person’s needs and preferences without considering the role that plays in community care. It can be challenging to take our experience with one patient’s journey and apply it to a larger group of patients with that same condition.
When the question of what we could have done differently arises out of a patient’s journey, it helps to consider the way other practitioners handle patients with similar issues. It is valuable to look at how we practice and how we manage common conditions, like diabetes, across a group of patients. It is useful to have tools that allow us to consider and measure how we could improve their care.
As family doctors, we have this information in our EMRs. What’s lacking, however, is the ability to collaborate with colleagues who are also sharing data, to look at trends in the community, and to compare and contrast with provincial or divisional aggregates. Sharing our data, safely and securely, can tell us about the care of our patients with various conditions, including diabetes. The data prompts us to ask, are we screening for diabetes? Are we monitoring the disease well?
Being part of the Health Data Coalition from the beginning, I have seen the positive impact data can make. I encourage my colleagues to register for HDC Discover, a GPSC-funded, physician-led, data-sharing application being used in clinics across the province.
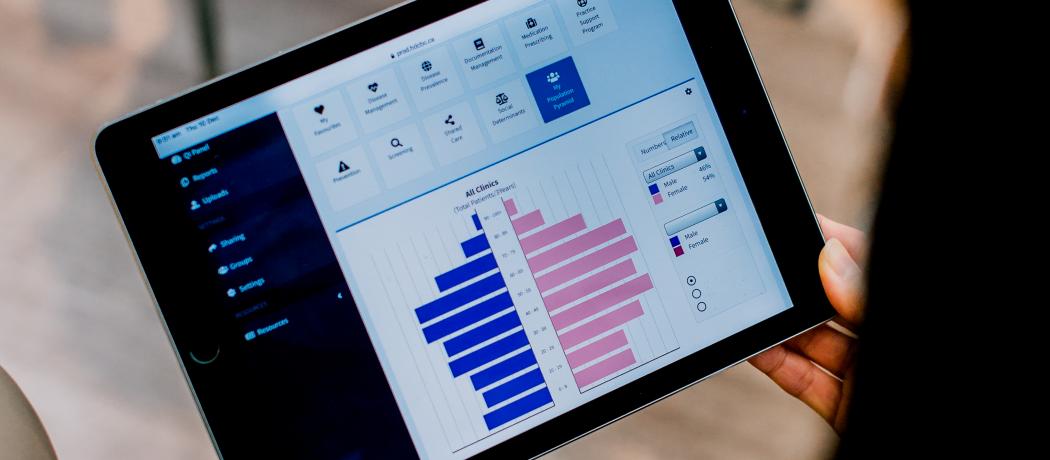
HDC Discover is a tool that allows us to look at information and anonymous EMR data to reflect, measure, and improve our practice. We are able to compare our treatment to other practices and changes and the impacts they have to the care we provide our patients, like Ms Harry.
Join physicians across BC using EMR data to help improve patient outcomes. Learn more about HDC Discover and enrol at www.hdcbc.ca/enrol.
—Bruce Hobson, MD
HDC Medical Director
* Ms Harry is a fictional, composite patient.
This post has not been peer reviewed by the BCMJ Editorial Board.